[ad_1]
Regulators on Friday approved two gene therapies for sickle cell disease that doctors hope could cure the painful, inherited blood disorder that affects mostly black people in the US.
The Food and Drug Administration said the one-time treatment can be used for patients 12 years of age and older with a severe form of the disease. One, made by Vertex Pharmaceuticals and CRISPR Therapeutics first approved therapy Based on CRISPR, the gene editing tool that won its inventor Nobel Prize in 2020. The second is made by Bluebird Bio and works differently.
“Sickle cell disease is a rare, debilitating and life-threatening blood disorder with a significant unmet need,” the FDA’s Dr. Nicole Verdun said in a statement announcing the approval. “We are especially excited to advance this field for individuals whose lives have been severely disrupted by this disease.”
Two gene therapies for sickle cell are approved in the US for the first time. The FDA has previously approved 15 gene therapies for other conditions. Some have list prices in the millions of dollars, and will also feature sickle cell therapy.
In the US, an estimated 1 in 100,000 people have sickle cell, and about one-fifth of them have the severe form. Sickle cell is most common in black people and 1 in 365 Nationally, black children are born with the disease. Scientists believe that being a carrier of the sickle cell trait helps protect against severe malaria, so the disease is more common in mosquito-prone areas like Africa or in people whose ancestors lived in those places.
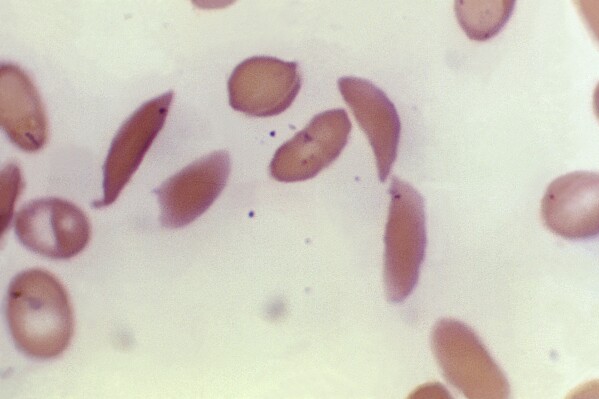
The disease affects hemoglobin, the protein in red blood cells that carries oxygen. The genetic mutation causes cells to become sickled or crescent-shaped, which can block blood flow, causing excruciating pain, organ damage, stroke and other problems.
Current treatments include medications and blood transfusions. The only permanent solution is a bone marrow transplant, which must come from a close-matched donor and brings the risk of rejection.
Gene therapy does not require a donor, which permanently alters the DNA in the patient’s blood cells. The goal of Vertex therapy, called CasGV, is to help the body return to the fetal form of hemoglobin that is present at birth — it is the adult form that is defective in people with sickle cell disease. CRISPR is used to knock out a gene in stem cells collected from a patient.
Bluebird’s treatment, called Lifegenia, aims to add copies of a modified gene that helps red blood cells produce “anti-sickling” hemoglobin that stops or reverses the deforming cells.
When patients receive treatment, stem cells are taken out of their blood and sent to the laboratory. Before the transformed cells can be reversed, they must undergo chemotherapy. This procedure requires at least two hospitalizations, one lasting four to six weeks.
Still, many patients say they would consider gene therapy given the severity of the disease.
Jalen Matthews, of Louisville, Kentucky, was diagnosed with sickle cell at birth and had her first pain at age 9. Three years later, the disease caused a spinal stroke, leaving him with some paralysis in his left arm and leg.
“I had to learn to walk again, feed myself, dress myself, basically learn to do everything again,” said Matthews, now 26.
Today, she keeps her sickle cell at bay by getting a blood transfusion every two months, in which five of her units of blood are replaced with healthy cells. She said gene therapy might be a better option and she plans to ask her doctor about it.
“A one-time treatment like this is sorely needed,” Matthews said.
The FDA approval is the first for Bluebird’s treatment; Vertex has been authorized before Britain And Bahrain.
Studies testing the treatments show that they work well. Of the 31 people treated in the Pivotal Vertex study with adequate follow-up, 29 were free of pain crisis for at least one year. In the Bluebird study, 28 of 32 patients had no severe pain or organ damage between six and 18 months after treatment.
But doctors say it has potential side effects and long-term consequences are unknown. For both, the required chemotherapy comes with risks such as infertility, hair loss and vulnerability to serious infections.
With Bluebird therapy, blood cancers have occurred, so the FDA said the label would include a “black box warning” about that risk. As with Vertex therapy, some scientists worry that CRISPR brings the possibility of “off-target effects,” which are unexpected changes to a person’s genome.
“It’s important to be cautious and optimistic about this therapy, but also know that there’s still a lot of experience with it,” said Dr. Benjamin Watkins, director of the pediatric stem cell and cell therapy program at Children’s Hospital New Orleans. Not there.” ,
Doctors said they do not expect every medical center to offer gene therapy because they require a lot of equipment and coordination among medical experts. They also don’t expect many people to find them right away. Watkins said some people may want to wait until more people get treatment.
Experts also warned that cost could be a barrier. The list price is $3.1 million for Bluebird Bio and $2.2 million for Vertex. How much patients pay will depend on insurance coverage and other factors. To help cover the costs, the U.S. Centers for Medicare & Medicaid Services announced A plan aimed at establishing partnerships with state Medicaid agencies and drug companies.
But ultimately, gene therapy “could be transformative and really change the landscape of sickle cell disease,” said Dr. Monica Bhatia, who treats children with the disease at NewYork-Presbyterian.
Matthews, who volunteers with The Sickle Cell Association of Kentuckiana, said she hopes the treatments will have a big impact.
“It’s a blessing,” she said. “This will really benefit all of us in the sickle cell community.”
,
The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Science and Educational Media Group. AP is solely responsible for all content.
[ad_2]
Source link